A layman’s explanation of PRP, OroGen Plus and Regenerative Medicine
By Bob Brandt, OroGen BioSciences
Platelets are the mediators of all wound healing. They regulate and modulate the rate of repair that the other healing cells perform. Think of them as the maestro leading the orchestra into a beautiful musical piece. First, he directs the horns to play. Then, he asks the strings to join in and all the time, regulating the flow, depth and tempo.
Now, because we have used so many platelets, the signal they send out is heard all over the body by a different subset of cells. Kind of like a construction crew…the plumbers, carpenters, electricians, bricklayers, painters, etc. They all have a specialty that is needed to construct a building. If we put a skeleton crew of construction workers at a job site, it takes quite a while for the job to be completed. Now if we increase the crew by tenfold, we hopefully can have our building up in a fraction of the time. The same is true with PRP and wound repair.
Now imagine this. Our construction crew is driving to work and the bridge that they have to cross to get to the job site collapsed during the night. They can all crawl down the embankment and up the other side to get to work, but it is going to take a very long time for them to get to their destination and they are going to have to expend a lot of energy to accomplish this. The same thing happens when we are trying to repair a torn ligament or tendon, broken bone, diabetic wound or possibly a spinal fusion. To a cell, looking over torn ligament fibers is akin to looking over the Grand Canyon. They will probably never get from one side of the fiber to the other, so the injury remains chronic and eventually, some scar tissue will form, but the fibers never mend themselves.
PRP Procedure
Our process uses the body’s own material to make a bridge so that the cells have somewhere to cross. We call this a matrix or scaffold and it contains not only fibrin but also vitronectin and fibronectin, in concentrated quantities, two very important proteins needed for wound healing. Inside of this matrix are the conductors, or the Pied Pipers, who are calling out to all the healing cells (including stem cells) in the body to come join the party at Fred’s injured leg. We have taken the simple and expanded on it to make it super juice in a way to make it easier and simpler to use. This is regenerative medicine!
So now apply this idea to Appearance Medicine and your face is repaired in the same manner. PRP is regenerative for healing wounds and skin…FABULOUS!!
The Course of PRP Treatment
10 to 20 minutes prior to treatment, your physician will draw 10 to 20 millilitres of your blood, using a standard procedure, causing minimal pain (like taking a standard blood test). Thereafter, he will separate the blood into its ingredients, in a procedure that will last 10-20 minutes. PRP is injected below the surface of the skin in the area of fat loss and/or wrinkles. It provides a gradual increase in skin thickness. Visible results appear after the first treatment session.
Treatment results will typically last up to (1-1½) years after the first treatment session in most patients. Touch-up treatments may be needed to maintain the desired effect.
Platelet counts are important for optimum results in treatment with Platelet Rich Plasma.
PRP (Platelet Rich Plasma) is a concentration of human platelets (PLT) in a small volume of plasma. PRP utilizes the patients own (autologous) PLT, derived from his/her blood.
Lasting Results
According to dozens of injections performed in the UK and Japan, 2-3 consecutive injections, performed within intervals of 1-3 months, will hold the skin rejuvenation effect for a minimum period of 12 months, as described in the seen in the scheme below.
- Promotes autologous local tissue growth and repair.
- The only filler that can regenerate wrinkles under the eyes.
- Patient’s safety – PRP is made out of patient’s own blood:
- No disease transmission.
- PRP is non-toxic
- No rejection with PRP
- Convenience – PRP is prepared at doctor´s office.
- Faster healing – PRP accelerates tissue synthesis
- Cost-effectiveness – No need for external substances.
- It is simple and easy to use.
- It is re-absorbed by the body in a few days.
More Technical Information About PRP
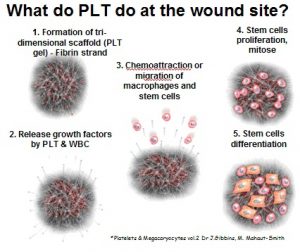
What does PLT do at the injection site?
- Form blood clots (“PLT gel”).
- Release Growth Factors and proteins (see below).
- Stimulate Stem Cells to regenerate new tissue.
- Accelerate bone healing through Osteo-progenitor cells.
PLT must be intact, in order not to damage these processes!!!
- PLT clotting occurs within 10 min after PLT de-granulation, thus anticoagulants in included within the PRP kit.
- The process of releasing growth factors (GF) from platelets is called de-granulation. During this process, the contents of the PLT -granules are being released by budding from PLT membranes and the addition of side chains. Thus, PLT is required to be viable and intact.
- GF bind to Receptors of the cells that are being attracted to the wound.
- Initiation of production of collagen and cell proliferation – Chemoattractant activity – attract Mesenchymal stem cells to the wound.
- Acceleration of the normal wound healing process.
Growth Factors and proteins released by PLT:
PDGF:
- Cells replication
- Stem cells differentiation
- Angiogenesis – vascularization
- Chemo-attraction of Macrophages, fibroblasts
TGF:
- Induction of connective tissue formation
ILGF:
- Wound healing
EGF:
- Induction of cell differentiation
- Fibrin
- Fibronectin
- Vitronectin
Contra-Indications
- Platelet Dysfunction Syndrome
- Critical Thrombocytopenia
- Hypofibrinogenaemia
- Haemodynamic Instability
- Sepsis
- Acute & Chronic Infections
- Chronic Liver Pathology
- Anti-coagulation Therapy
Suggested Applications:
- Subcision technique (acne scars)
- Layer-specific transplant
- “Tenting” of skin
- “Cul-de-sac” & needle bevel up
- Over-correction 50%
- Avoid “under-dosing”
- Serial Rx’s = accumulative effect
- Minimal-trauma technique (long needle)
Intra-dermal injection = blanching
PRP FAQs?
Why is there excitement about PRP?
PRP usage takes advantage of normal the body´s healing pathways, only at an accelerated rate. During wound healing, many cells rush into the wound site. Among these cells, there are platelets (PLT).


